One thing people might not know about Parkinson’s is how difficult it is to diagnose. The early symptoms of Parkinson’s—shakiness, muscle stiffness, impaired balance, and depression—are common to myriad illnesses and begin incrementally. In 2011, my partner, Greg, became aware of his right hand trembling when a co-worker pointed it out. Greg sought medical advice and ended up at the neurology department of the University of Pittsburgh Medical Center (UPMC). His diagnosis at the time was “Parkinson’s-like symptoms.” The neurologist said the shaking could be benign essential tremors, or Greg could have something more serious, like Multiple Symptom Atrophy or Supernuclear Palsy, debilitating diseases. The cause of Greg’s tremors would only become clear as time passed, and symptoms were observed.
Greg added a local neurologist, Dr. David Libell of West Virginia University Hospitals (WVUH), to his circle of physicians. He checked in with Dr. Libell once a year. By the time we started dating in 2015, Greg’s tremor was apparent part of the time, but his symptoms were progressing slowly. He was still active in all areas of life, employed fulltime by the Federal Bureau of Prisons; he was still climbing on the roof when a gutter came loose in a storm and still gung-ho for weed eating, golfing, and pitching a canopy tent by the river for concerts at Palatine Park.
In 2017, when it came time for his annual appointment with Dr. Libell, Greg asked me to accompany him. It had been six years since Greg’s first awareness of his tremor, and some of his symptoms were becoming more bothersome. He didn’t like the shuffle in his step, and his fine motor skills were deteriorating. He could no longer grasp a toothbrush and had trouble turning a key in a lock and buckling his seat belt. The tremors on his right side occurred more frequently, like when he relaxed watching TV, and his foot tapped to invisible music.
Dr. Libell suggested it was time to begin carbidopa levodopa, a drug that addresses dopamine loss, though Greg was still not officially diagnosed with Parkinson’s. Dr. Libell prescribed a low dose of carbidopa levodopa three times a day at regular intervals, and the dose could be adjusted based on results. I pointed out that regular intervals weren’t part of our daily routine. Sometimes Greg slept in late; sometimes he was up when the rooster crowed. He stayed up past midnight or was tucked in by eight. By then, Greg had retired from the Bureau after twenty-two years of service, in part due to his worsening symptoms. Retirement freed him and decreased his anxiety significantly, though he still took an anti-depressant since depression is part of Parkinson’s.
Greg attempted to follow the doctor’s instructions. He sat an alarm on his phone that went off three times a day, morning, noon, and night, to remind him to take his levodopa. The alarm played a cheerful song that lasted a billion-gazillion seconds. He left his phone all over the house, and he slept through the alarm more times than I can count, or he wasn’t even home when the alarm went off. He refused to commit to taking levodopa as prescribed. He said the drug didn’t work, and it nauseated and fatigued him. I couldn’t argue with his experience, though I’ll admit to thinking if he took levodopa at regular intervals, we’d be better able to assess its effectiveness. He eventually turned the phone alarm off and took his levodopa sporadically. We lived with his symptoms in relative peace and silence for the next couple of years.
By 2019, Greg’s tremors were more pronounced, and other symptoms had progressed. When he relaxed watching TV or resting, his glute muscles clenched up and refused to release. His balance was worse, and he fell a couple of times. Sometimes when he was driving, his foot would tremor on the gas pedal. At his annual visit with Dr. Libell, Greg asked the physician for a definite diagnosis of Parkinson’s in order to explore other treatment like deep brain stimulation surgery or possibly long-term disability.
“I can’t diagnose you with Parkinson’s,” Libell said. “I’m only a neurologist.” The line became a running joke between Greg and me. I’d ask him to take out the garbage, and he’d say, “I can’t. I’m only a neurologist.”
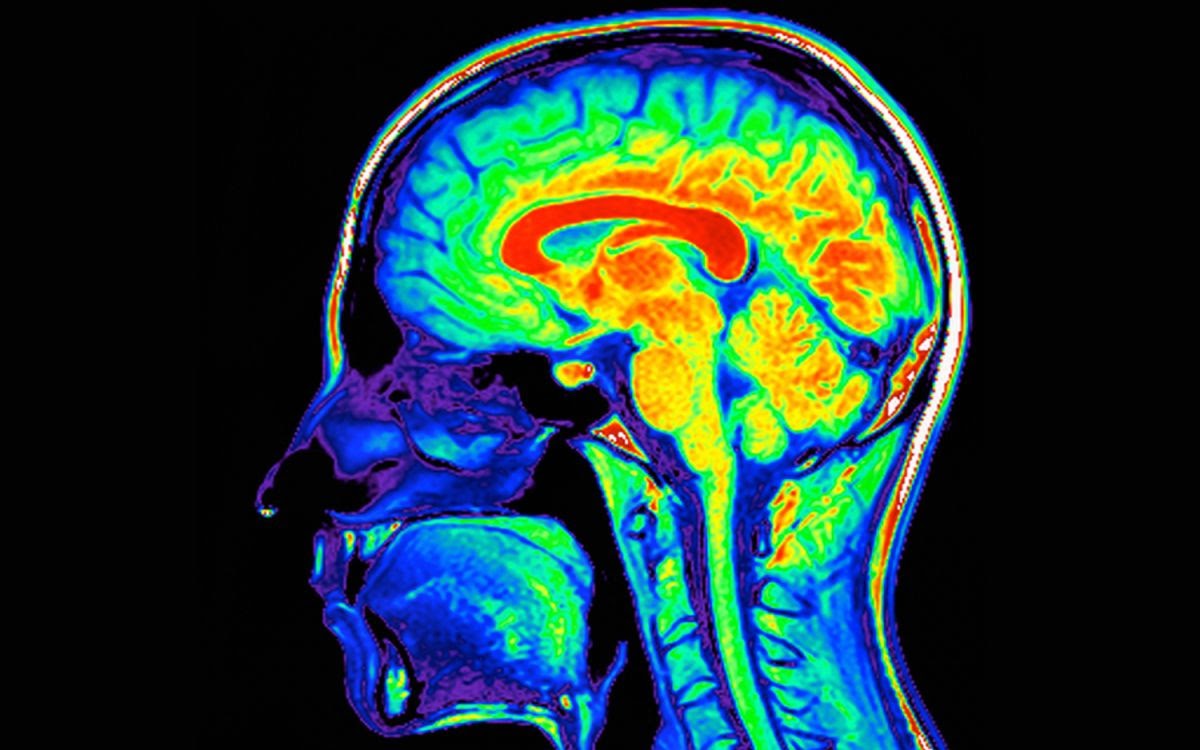
Dr. Libell told us only a movement disorders specialist could issue a definite Parkinson’s diagnosis. The nearest specialist to us was at Cabell Huntington Hospital in Huntington, West Virginia, a facility about three hours away. We made the appointment and went for a consultation with Dr. Suresh G. Kumar. In order to confirm a Parkinson’s diagnosis, Greg would need to undergo a DaT scan, a day-long outpatient procedure that involves a chemical injected into a vein and destined for the brain, which is imaged using single photo emission computerized tomography, or SPECT scanning. The scan produces an image of the brain lit up with primary colors: red, yellow, blue. Greg underwent a DaT scan in early 2020, just before the Covid pandemic began. The test confirmed that Greg had Parkinson’s, his brain a map of colors as bright as a kindergartner’s drawing.
The pandemic slowed down our quest for effective treatment, and gave Greg time to research his options, which were few, as there is no cure for Parkinson’s at this time. The two treatments that attracted his interest were MR-guided focused ultrasound and deep brain stimulation (DBS) surgery. Ultrasound was much less invasive than surgery and involved ablating a small spot on the brain to reduce tremors. In late 2020, Greg was finally able to make an appointment at the WVU Rockefeller Neuroscience Institute, and we were hopeful we could find a therapy to alleviate his symptoms.
The appointment was an education. We discovered ultrasound wasn’t recommended for Greg’s particular case. The ablation was irreversible and would only treat tremors and muscle rigidity on one side of his body. DBS, it turned out, was his only option, and Greg decided to begin the months-long process that would lead to brain surgery.
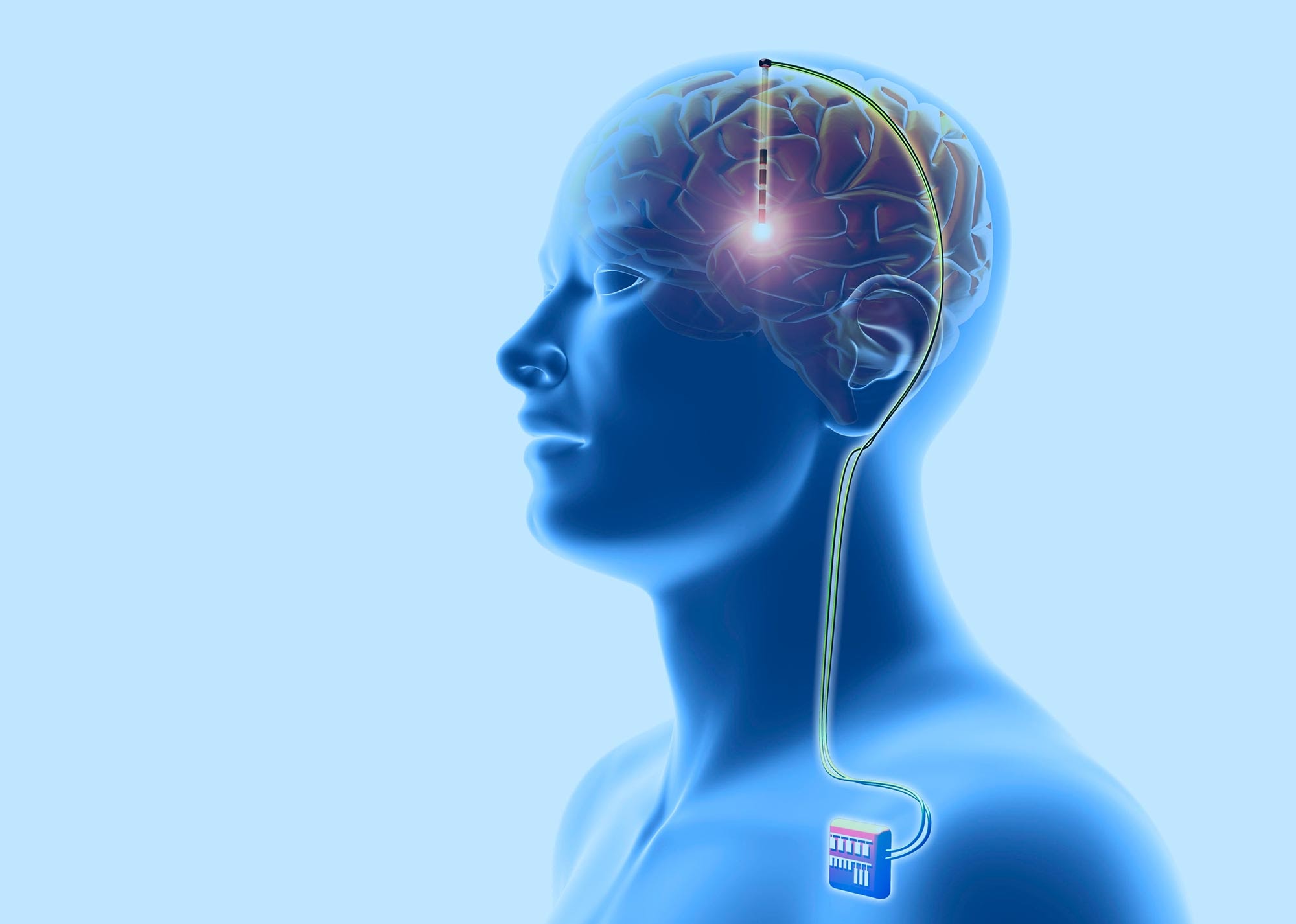
The first step was a string of evaluations: cognitive, physical, and psychological. Once he cleared those, more invasive procedures were scheduled at two-week intervals. The first surgery implanted four screws in his skull; the screws would hold a basket-like metal helmet in place during the second surgery, which would determine where to embed electrodes in his brain. During this surgery, Dr. Brandmeir hooked up the juice to the electrodes and asked Greg to perform simple tasks, like raising one finger or lifting his arm. When I asked Greg for details to write this essay, he said, “I remember it felt good because the tremors were gone.” After determining the electrodes were located correctly, Dr. Brandmeir turned the juice off. During the third surgery, the surgeon implanted a battery in Greg’s chest (in the same place pacemakers are generally located) and ran wires under his skin from the battery to the electrodes in his head. Four weeks later, once all the incisions were healed, Greg met with a team of medical technicians to program the DBS system. On July 14, 2021, he became a successful DBS patient.
I’m thankful this Thanksgiving season to report Greg’s DBS surgery was a success. His tremor is significantly reduced, his muscles don’t seize up, and his sense of balance is improved. Of course, he’ll have to maintenance his implants for life. The month after the final surgery, he wasn’t allowed to travel in case complications developed. Around the five-year mark, he’ll have to have another surgery to replace the battery in his chest. He’s returned twice to the WVU Rockefeller Neuroscience Institute to get “tuned up,” as he calls it. At his last “tune-up” appointment, the medical technician adjusted Greg’s equipment in a way that actually brightened his outlook and mood. It happens that tinkering with the brain tinkers with the emotions, and DBS can provide treatment for lifelong depression and addiction. There are even articles about DBS that raise the question: Can a person be too happy? Can a person be so happy they lose touch with reality?
Greg’s not that happy. I make sure of that, me and the daily news. I remind him when to take out the trash and yell at him for misplacing his phone again, but it’s Senator Joe Manchin and his obstructionist politics that really raise Greg’s blood pressure. He has a passion for politics, our collective grandchildren, and the community that surrounds us. DBS surgery allows Greg to live with his Parkinson’s and enjoy everyday life on his own terms.
Categories: Health, Suzanne's Voice